A health care worker at a drive-through site in Greenville, Miss., administers a COVID-19 vaccine shot in January. Mississippi was one of the first states to add a body mass index of 30 or more (a rough gauge of obesity) to its current list of qualifying medical conditions for vaccine eligibility.
Rory Doyle/Bloomberg via Getty Images
hide caption
toggle caption
Rory Doyle/Bloomberg via Getty Images
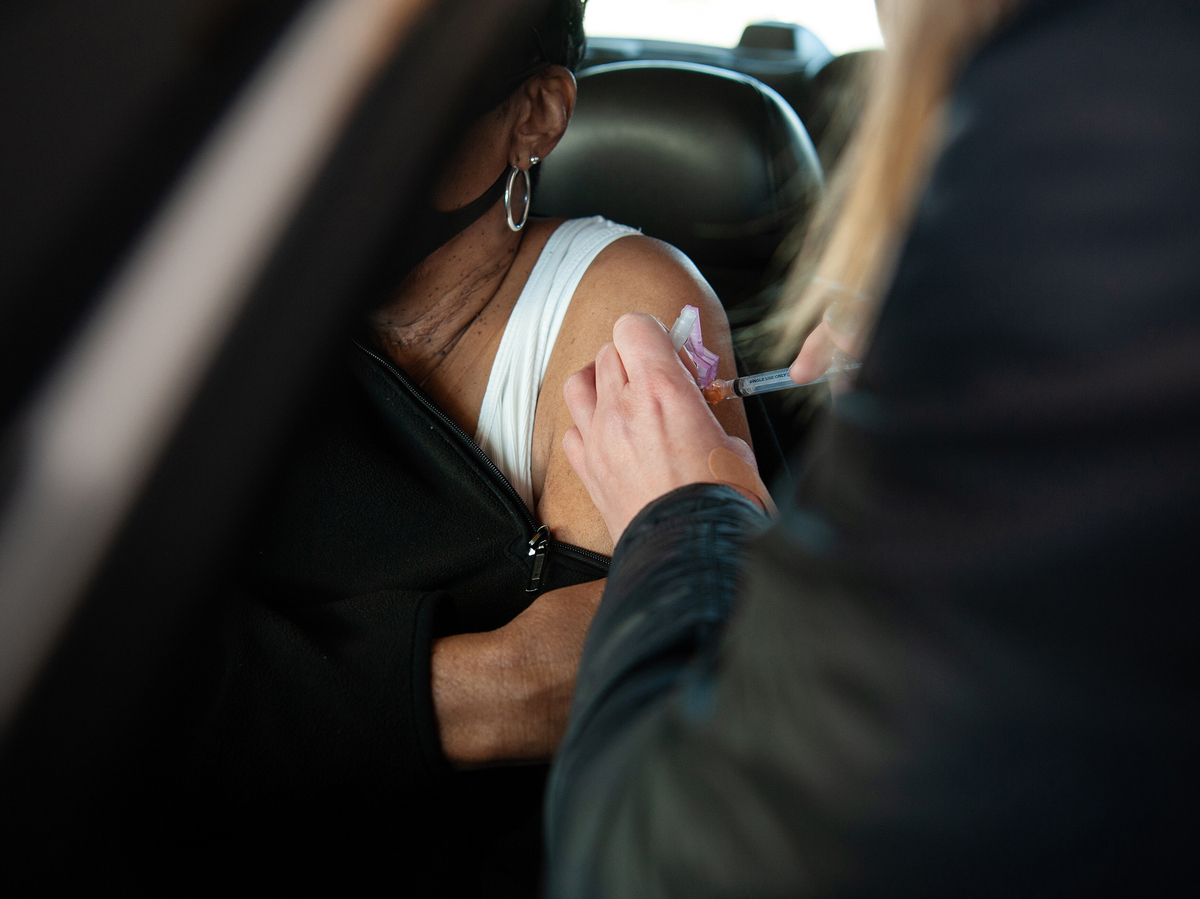
A health care worker at a drive-through site in Greenville, Miss., administers a COVID-19 vaccine shot in January. Mississippi was one of the first states to add a body mass index of 30 or more (a rough gauge of obesity) to its current list of qualifying medical conditions for vaccine eligibility.
Rory Doyle/Bloomberg via Getty Images
In January, as Mississippi health officials planned for their incoming shipments of COVID-19 vaccines, they assessed the state’s most vulnerable: health care workers, of course, and elderly people in nursing homes. But among those who needed urgent protection from the coronavirus ripping across the Magnolia State were 1 million Mississippians with obesity.
Obesity and weight-related illnesses have been deadly liabilities in the COVID-19 era. A report released this month by the World Obesity Federation found that increased body weight is the second-greatest predictor of COVID-19-related hospitalization and death across the globe, trailing only old age as a risk factor.
As a fixture of life in much of America, especially in the American South — home to nine of the nation’s 12 heaviest states — obesity is playing a role not only in COVID-19 outcomes but in the calculus of the vaccination rollout.


Mississippi was one of the first states to add a body mass index of 30 or more (a rough gauge of obesity tied to height and weight) to the list of qualifying medical conditions for the shots. About 40% of the state’s adults meet that definition, according to federal health survey data, and combined with the risk group already eligible for vaccination — residents 65 and older — that means fully half of Mississippi’s adults are entitled to vie for a restricted allotment of shots.
At least 29 states have greenlighted obesity for inclusion in the first phases of the vaccine rollout. That’s a vast widening of eligibility that has the potential to overwhelm government efforts to distribute vaccines in those states and to heighten competition for scarce doses.
“We have a lifesaving intervention, and we don’t have enough of it,” says Jen Kates, director of global health and HIV policy for the Kaiser Family Foundation. “Hard choices are being made about who should go first, and there is no right answer.”


The sheer prevalence of obesity in the nation was a public health concern long before the coronavirus pandemic — 2 in 3 Americans exceed what is considered a healthy weight, with 42% falling into the obesity range, according to the Centers for Disease Control and Prevention. But COVID-19 dramatically fast-tracked the discussion from warnings about the long-term damage that excess fat tissue can pose to heart, lung and metabolic functions to far more immediate threats.
In the United Kingdom, for example, overweight COVID-19 patients (defined as people who have a BMI between 25 and 30) were 67% more likely to require intensive care, and obese patients three times likelier, according to the World Obesity Federation report. A CDC study released Monday found a similar trend among U.S. patients and noted that the risk of hospitalization, ventilation and death related to COVID-19 increased with patients’ obesity level.
The counties that hug the southern Mississippi River are home to some of the most concentrated pockets of extreme obesity in the United States. Coronavirus infections began surging in Southern states early last summer, and hospitalizations rose in step.
Over the course of the pandemic, deaths linked to COVID-19 in rural stretches of Mississippi, Tennessee, Louisiana and Arkansas have been overshadowed by the sheer number of such deaths in metropolitan areas like New York City, Los Angeles and Essex County, N.J. But the coronavirus has been similarly unsparing in many Southern communities as a share of the population there. In sparsely populated Claiborne County, Miss., on the flood plains of the Mississippi River, 30 residents — about 1 in 300 — had died of a coronavirus-related infection as of early March. East Feliciana Parish, La., north of Baton Rouge, had lost about 1 in 180 residents to COVID-19 by then — 106 deaths.
“It’s just math,” says Dr. James de Lemos, a professor of internal medicine at UT Southwestern Medical Center in Dallas, who led a study of hospitalized COVID-19 patients published in the medical journal Circulation late last year. “If the population is more obese and obesity clearly contributes to worse outcomes, then neighborhoods, cities, states and countries that are more obese will have a greater toll from COVID.”

And because in the U.S. obesity rates tend to be relatively high among African Americans and Latinos who are poor and have diminished access to health care, “it’s a triple whammy” in those communities, de Lemos says. “All these things intersect.”
Poverty and limited access to medical care are common in the South, where residents like Michelle Antonyshyn, a former registered nurse and mother of seven in Salem, Ark., say they are afraid of the virus. Antonyshyn, 49, has obesity and debilitating pain in her knees and back, though she does not have high blood pressure or diabetes, two underlying conditions that federal health officials have determined are added risk factors for severe cases of COVID-19.
Still, Antonyshyn says, she “was very concerned just knowing that being obese puts you more at risk for bad outcomes such as being on a ventilator and death.” As a precaution, Antonyshyn says, she and her family locked down early and stopped attending church services in person, participating online instead.
“It’s not the same as having fellowship, but the risk for me was enough,” says Antonyshyn.
Governors throughout the South seem to recognize that weight can contribute to COVID-19 complications and have pushed for vaccine eligibility rules that prioritize obesity. But on the ground, local health officials are girding for having to tell newly eligible people who qualify as obese that, even so, there aren’t enough shots to go around yet.


In Port Gibson, Miss., Dr. Mheja Williams, medical director of the Claiborne County Family Health Center, has been receiving barely enough doses to inoculate the health workers and oldest seniors in her county of 9,600. One week in early February, she received 100 doses.
Obesity and extreme obesity are endemic in Claiborne County, and that means residents often don’t recognize their weight as a risk factor, whether for COVID-19 or other health issues, physicians say. Those risks are exacerbated, Williams notes, by middle-aged and younger residents in the area who tend not to be especially vigilant about following the CDC’s pandemic guidance on physical distancing. Mask use, she adds, is rare.
The rise of obesity in the U.S. over the past half-century has been well documented, as the nation turned from a diet of fruits, vegetables and limited meats to one laden with ultraprocessed foods and rich with tasty salt, fat, sugar and artificial flavorings, along with copious amounts of meat, fast food and soda. The U.S. has been among the leaders of the global obesity race, setting records as even toddlers and young children grew implausibly, dangerously overweight.
Well before COVID-19, obesity was a leading cause of preventable death in the United States. In 1998, the National Institutes of Health declared it a disease, one that fosters heart disease, stroke, Type 2 diabetes and breast, colon and other cancers.
Researchers say it is no coincidence that nations like the U.S., the U.K. and Italy, with relatively high obesity rates, have proved particularly vulnerable to the novel coronavirus.
They believe the virus may exploit underlying metabolic and physiological impairments that often exist in concert with obesity. Extra fat can lead to a cascade of metabolic disruptions, chronic systemic inflammation and hormonal dysregulation that may thwart the body’s response to infection.
Other respiratory viruses, like the influenza virus and the virus that causes SARS, which appeared in China in 2002, rely on cholesterol to spread enveloped RNA virus to neighboring cells, and researchers have proposed that a similar mechanism may play a role in the spread of the coronavirus that causes COVID-19.
There are also practical problems for coronavirus patients with obesity who are admitted to the hospital. They can be more difficult to intubate because of excess central weight pressing down on the diaphragm, making breathing with infected lungs even more difficult.
Physicians who specialize in treating patients with obesity say public health officials need to be more forthright and urgent in their messaging as they telegraph the risks of this COVID-19 era.
“It should be explicit and direct,” says Dr. Fatima Stanford, an obesity medicine specialist at Massachusetts General Hospital and a Harvard Medical School instructor.
Stanford denounces the fat-shaming and bullying that people with obesity often experience. But telling patients, as well as the public, that obesity increases the risk of hospitalization and death from a coronavirus infection is crucial, she says.
“I don’t think it’s stigmatizing,” Stanford says. “If you tell them in that way: It’s not to scare you — it’s just giving information. Sometimes people are just unaware.”
Kaiser Health News produces in-depth journalism about health policy issues. Together with policy analysis and polling, KHN is one of the three major programs of the Kaiser Family Foundation, an endowed nonprofit, and is not affiliated with Kaiser Permanente.
